A patient presented with maxillary anterior teeth exhibiting reduced incisal length and sought esthetic enhancement through a minimally invasive, no-preparation approach. Six ultra-thin zirconia veneers were fabricated using Projection Micro Stereolithography (PµSL) technology, transitioning the patient’s shade from A1 to OM3. The final outcome demonstrated increased tooth length, improved brightness, and a natural appearance. This case highlights the potential of additive, ultra-thin zirconia veneers to achieve predictable esthetic enhancement while preserving enamel.
Case Study
Additive Six-Unit Anterior Esthetic Rehabilitation Utilizing Ultra-Thin Zirconia Veneers
Developed by UltraThineer, In collaboration with Dr. Anatoly Bensianoff, DDS, Magic Smile Dental
Introduction
Reduced incisal length in the maxillary anterior teeth can pose both functional and esthetic challenges, affecting smile harmony, phonetics, and anterior guidance. Patients increasingly prefer conservative restorative options that enhance tooth length and esthetics while preserving enamel. Traditional porcelain veneers often require significant tooth reduction, which may conflict with the goals of minimally invasive dentistry. Ultra-thin zirconia veneers offer a predictable, additive approach, combining high strength with minimal thickness. This case report presents the use of ultra-thin zirconia veneers to restore incisal length and improve smile esthetics in a conservative, digitally guided manner.
Case Presentation
The patient presented to Magic Smile Dental in Linden, New Jersey seeking longer, brighter anterior teeth without conventional preparation. Dr. Anatoliy Bensianoff collaborated with the UltraThineer team to develop a conservative, additive treatment plan. Six 120µm ultra-thin zirconia veneers for teeth #6–11 were fabricated using PµSL technology, and the patient’s shade was transitioned from A1 to OM3. Multiple design iterations ensured optimal tooth length, brightness, and natural appearance. The final restorations demonstrated successful esthetic enhancement while preserving enamel.
Chief Complaint:
The patient presented with a primary concern that their front teeth appear shorter and expressed a desire to address this issue.
Clinical Findings:
Clinical examination revealed worn incisal edges on the upper anterior teeth.
Diagnosis:
Tooth attrition secondary to parafunctional habits.
Treatment Plan
A comprehensive case history was obtained, including medical and dental history, esthetic concerns, and patient expectations. Preoperative records included intraoral and extraoral photography, radiographic imaging, intraoral scanning, and a detailed clinical examination to assess tooth proportions, incisal length, and occlusion. After reviewing the patient’s esthetic goals, the digital records were submitted to the UltraThineer team to initiate the restorative design and 3D printing process. The patient expressed a desire for a more squared tooth shape with defined canines to maintain a natural, harmonious appearance, while transitioning to a bright “Hollywood” white shade. A collaborative design process was employed, involving multiple iterations between Dr. Anatoly Bensianoff and the UltraThineer team. Modifications focused on achieving ideal incisal length, tooth width-to-height ratios, and incisal edge morphology, ensuring the restorations complemented the patient’s smile while preserving maximum enamel. The finalized design incorporated six ultra-thin veneers for teeth #6–11, fabricated at 120µm (0.12mm).
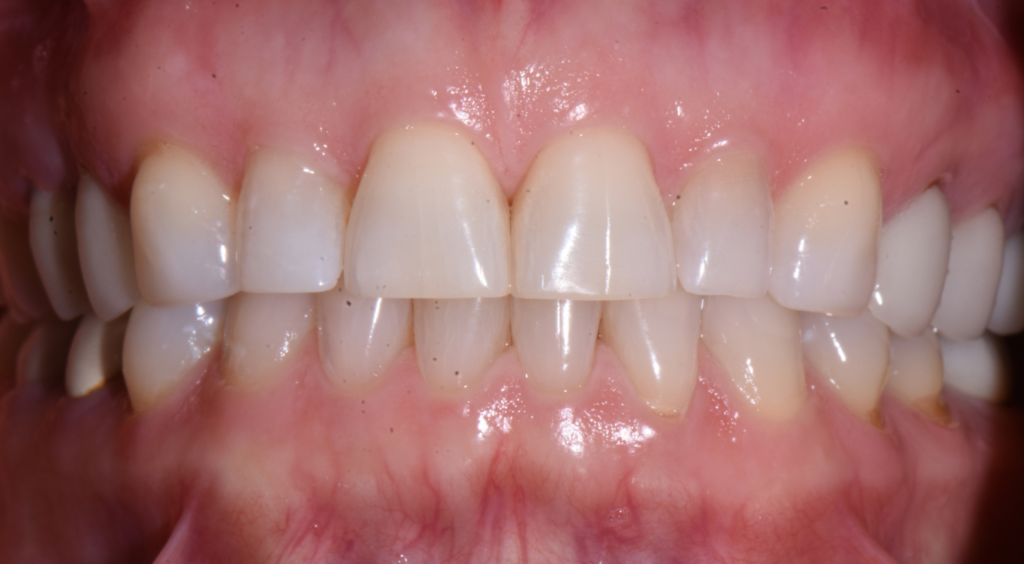
Fig 1
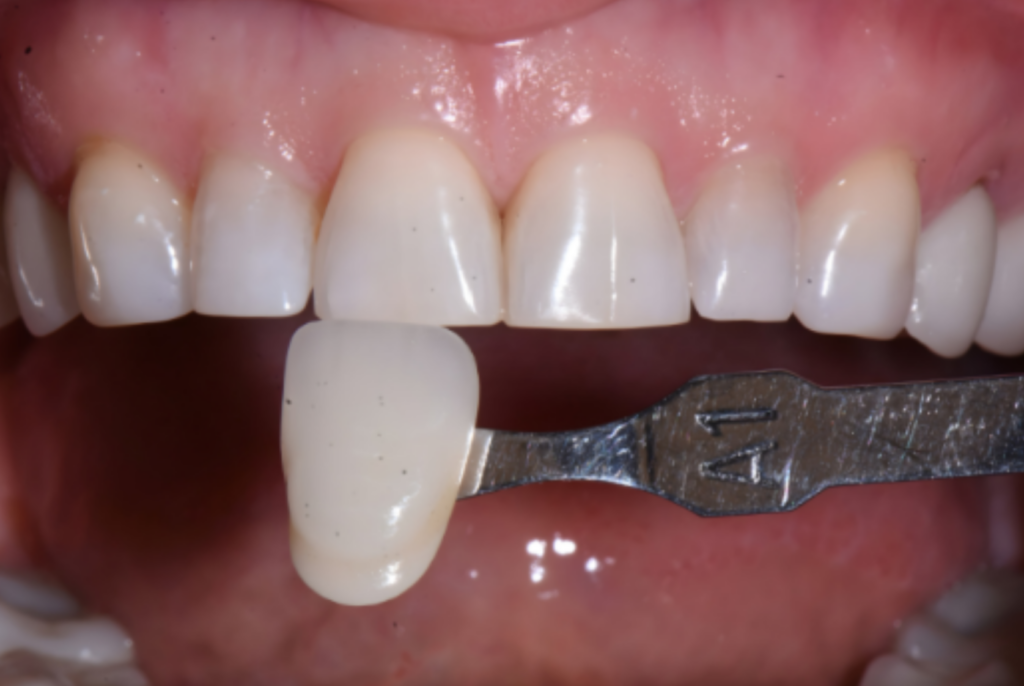
Fig 2
Fig 3
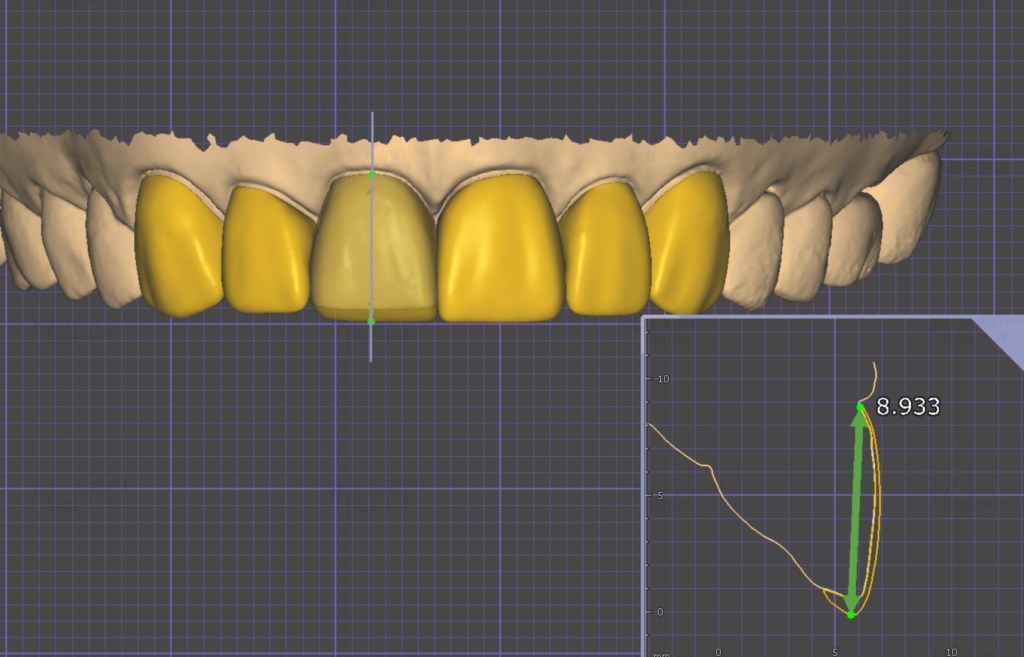
Fig 4
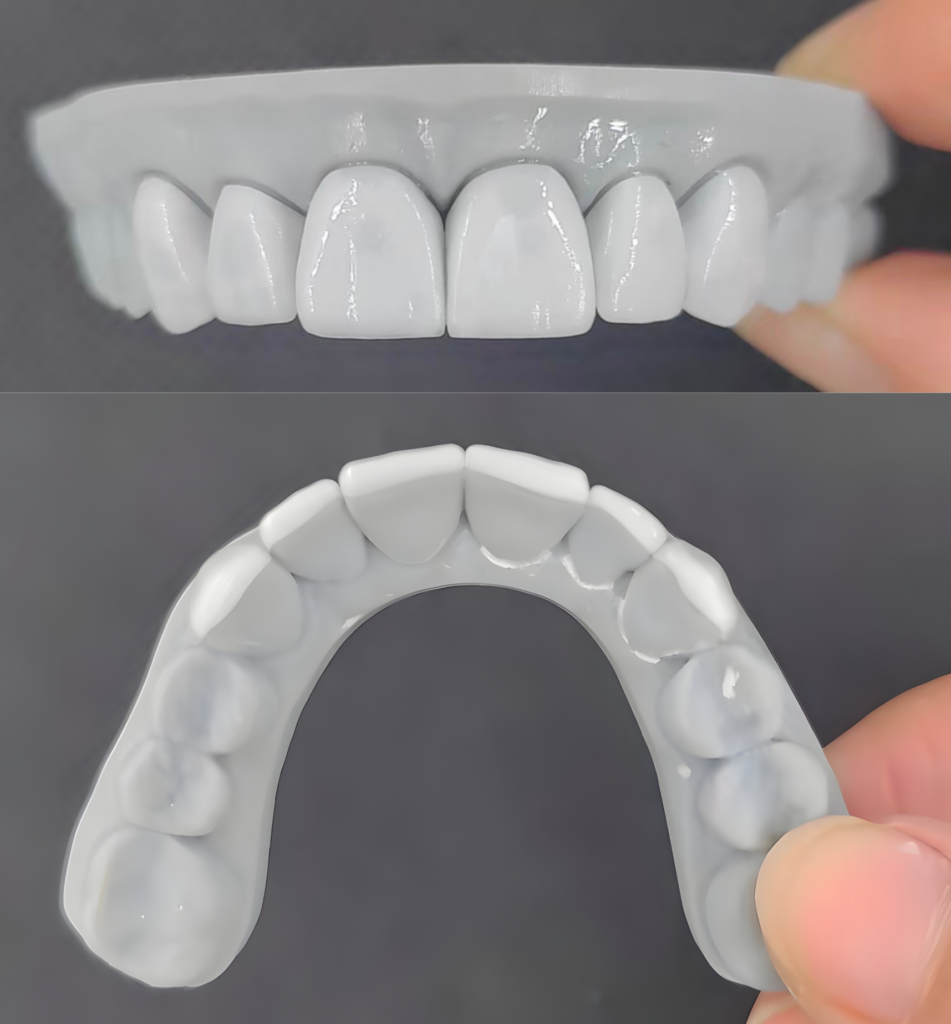
Fig 5
Treatment Procedure
The treatment began with a test fit of the veneers then cleaned in an ultrasonic bath for 3 minutes and air dried. Next, 9.5% hydrofluoric acid was applied precisely for 60 seconds, including the margins, followed by another 3-minute ultrasonic cleaning. Two layers of porcelain primer (silane) were brushed onto the veneers, allowed to sit for 5 minutes, then air dried for 30 seconds. A thin layer of porcelain bonding resin was applied without light curing. The veneers were preloaded with permanent cement and protected under an orange shield after being warmed in the composite warmer. On the tooth surfaces, a plaque indicator was applied followed by fluoride-free pumicing and micro etching with 32% phosphoric acid. The teeth were then etched with 32% phosphoric acid for 30 seconds, rinsed thoroughly for 30 seconds, and 1 to 2 thin layers of All-Bond Universal adhesive were applied, air thinned, and light cured for a minimum of 10 seconds at 800mW/cm2. The veneers were seated and tack-cured in place to stabilize positioning. Excess uncured cement was then carefully removed prior to final curing as cured cement is highly difficult to remove, especially interproximally. Once excess cement was removed, the veneers were light cured for 20 seconds. A 12-blade scalpel, interproximal saws, and scalers were used to remove any residual cement. Glycerin was then placed over the margins to prevent oxygen inhibition, and a final 20 second cure was done. After rinsing the glycerin, contacts and occlusion were checked, and final radiographs were taken.
Outcome and Follow-Up
The six ultra-thin zirconia veneers were successfully placed on teeth #6–11, achieving the patient’s desired esthetic goals. Postoperative evaluation demonstrated enhanced incisal length, improved tooth brightness, and a harmonious, natural appearance. The patient was highly satisfied with the overall outcome, noting both the subtlety of the additive enhancements and the dramatic improvement in smile esthetics.
Follow-up assessments were performed at 2 weeks and 2 months post-placement to evaluate fit, occlusion, and soft tissue response. No complications or sensitivity were reported, and the veneers maintained excellent marginal adaptation and surface integrity. The patient was instructed on routine oral hygiene and maintenance to ensure long-term durability of the restorations.
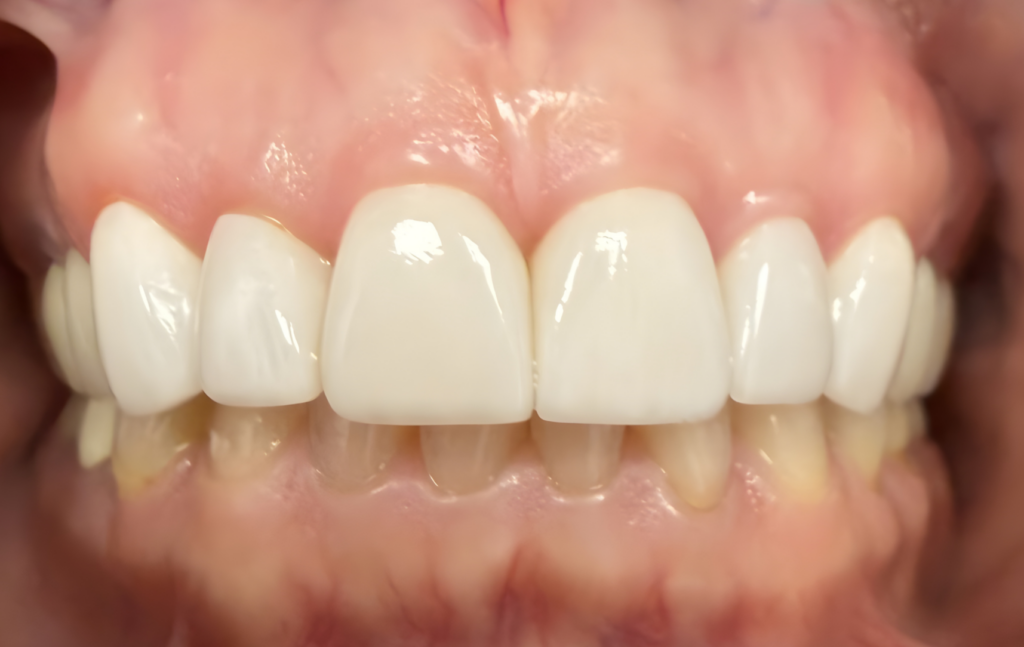
Fig 6
Fig 7
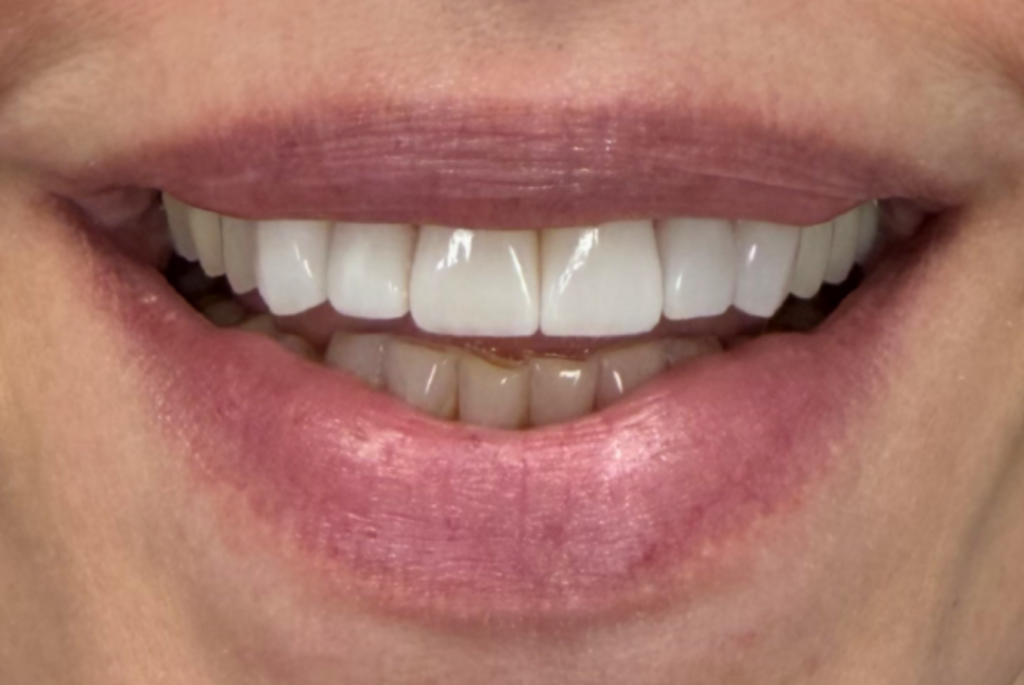
Fig 8
Discussion
Six ultra-thin zirconia veneers fabricated at approximately 120µm (0.12mm) thick enabled incisal length and esthetic improvement without conventional tooth preparation. The incorporation of a digital workflow further enhanced treatment precision. Intraoral scanning, photographic analysis, and digital design allowed for careful evaluation of tooth proportions, incisal edge position, and overall smile harmony prior to fabrication. Close collaboration between the clinician and UltraThineer enabled multiple refinements to the proposed restorations, ensuring that the final design met the patient’s esthetic goals.
Advances in ceramic manufacturing technologies, including Projection Micro Stereolithography (PµSL), have expanded the clinical applications of zirconia. This technology enables fabrication of restorations at significantly reduced thickness while maintaining the material’s favorable mechanical properties, including high flexural strength and fracture resistance. As demonstrated in this case, these characteristics allow zirconia to function effectively in ultra-thin veneer applications that rely on an additive treatment philosophy.
The clinical outcome illustrates that modest additive changes in incisal length, tooth proportions, and shade can produce substantial improvements in smile esthetics. Transitioning from shade A1 to OM3, combined with optimized incisal morphology, achieved the patient’s desired enhancement while maintaining a natural appearance. Short-term follow-up evaluations confirmed stable marginal adaptation, healthy soft tissue response, and high patient satisfaction.
Conclusion
This case report demonstrates that UltraThineer zirconia veneers can provide an effective and minimally invasive solution for improving anterior esthetics. By preserving enamel and integrating digital design with advanced ceramic manufacturing techniques, clinicians can achieve predictable esthetic outcomes while minimizing biological cost. The successful rehabilitation of teeth #6–11 in this case restored incisal length, enhanced brightness, and improved smile harmony without conventional tooth preparation. Ultra-thin zirconia veneers fabricated through modern additive technologies represent the future in conservative esthetic dentistry.
References
- Denry I, Kelly JR. State of the art of zirconia for dental applications. Dent Mater. 2008;24(3):299-307.
- Magne P, Belser UC. Bonded porcelain restorations in the anterior dentition: a biomimetic approach. Chicago: Quintessence Publishing; 2002.
- Kelly JR, Denry I. Stabilized zirconia as a structural ceramic: an overview. Dent Mater. 2008;24(3):289–298.
