Minimally invasive restorative dentistry prioritizes the preservation of natural tooth structure while achieving esthetic improvement. This case report presents the selective rehabilitation of the maxillary central incisors using no-prep zirconia veneers. The patient sought a subtle enhancement in shade and surface texture without altering tooth shape, alignment, or overall smile architecture. Two 80µm (.08mm) ultra-thin, 3D-printed zirconia veneers were fabricated and placed on teeth #8 and #9. Careful treatment planning and material selection allowed for improved brightness and surface uniformity while maintaining the patient’s natural proportions and incisal characteristics. The outcome demonstrates that conservative veneer therapy limited to the central incisors can deliver noticeable esthetic improvement while preserving enamel, minimizing chair time, and maintaining the integrity of the existing smile.
Case Study
Targeted Esthetic Enhancement with Minimal Intervention Using UltraThineer
Developed by UltraThineer, In collaboration with Dr. Tai Ha, DDS, Newport Beach Dental Studio
Introduction
In this case, the primary esthetic concern was to harmonize the shade of the maxillary central incisors with the adjacent lateral incisors (teeth #7 and #10) while maintaining the original tooth shape and smile architecture. Given the patient’s desire for minimal intervention, a no-prep approach was selected to allow for conservative correction of shade discrepancies without compromising enamel or altering existing contours. This report highlights how minimal, carefully planned changes to the central incisors can produce noticeable yet natural esthetic improvement while preserving the integrity of the patient’s smile.
Case Presentation
After clinical evaluation, Dr. Tai Ha of Newport Beach Dental Studio in Newport Beach, California, contacted UltraThineer to address the patient’s esthetic concerns. The patient sought a uniform smile without alteration of tooth morphology. Dr. Ha selected UltraThineer no-preparation, 80μm (.08mm) 3D printed zirconia veneers to achieve optimal shade match and esthetic outcomes while preserving enamel integrity.
Chief Complaint:
Patient presented with primary concerns regarding the opacity and visible white spot lesions affecting the maxillary central incisors, seeking esthetic improvement.
Clinical Findings:
Clinical examination revealed localized enamel demineralization presenting white spot lesions, as well as areas of excessive translucency that did not harmonize with adjacent teeth.
Diagnosis:
Enamel demineralization.
Treatment Plan
A comprehensive case history was obtained, followed by pre-operative photography, radiographic imaging, intraoral scanning, and a detailed clinical examination. After a thorough discussion of the patient’s aesthetic goals, the digital records were submitted to UltraThineer for case design and initiation of the 3D printing process. The patient expressed that she did not want any additional length added to her teeth. Her primary objective was to shade-match the maxillary central incisors to the adjacent lateral incisors (teeth #7 and #10) to achieve uniformity across the upper arch. She was adamant about maintaining her natural tooth shape and requested the thinnest veneer possible to preserve the existingstructure. The treatment plan included two maxillary veneers. The patient’s existing tooth shade ranged from BL3 to BL1, with BL1 selected as the final shade to achieve a uniform shade match. From a functional standpoint, no modifications were required.
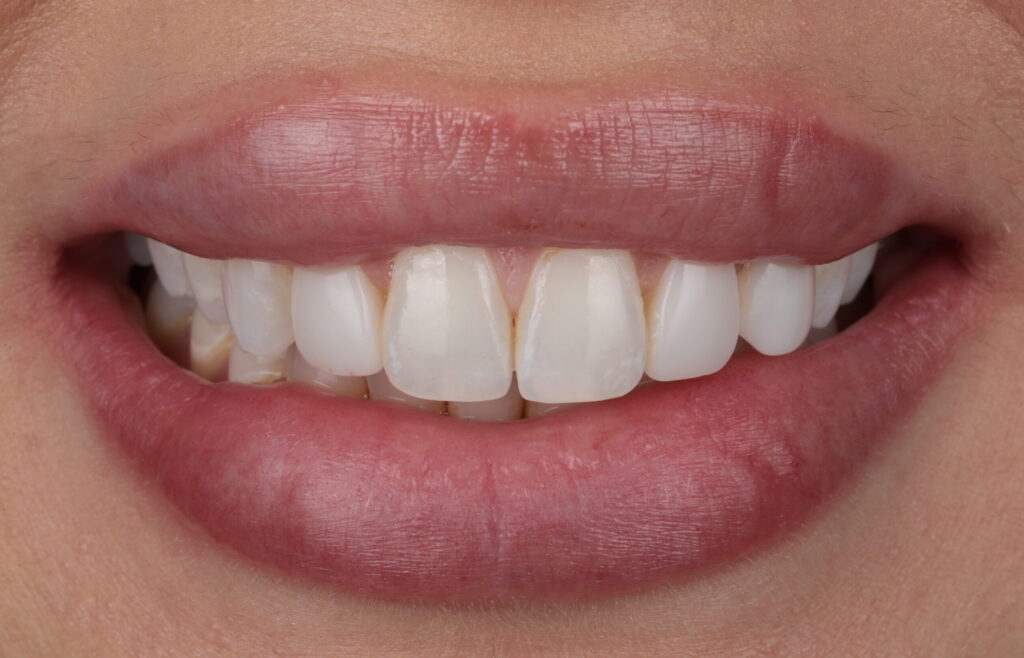
Fig 1
Fig 2
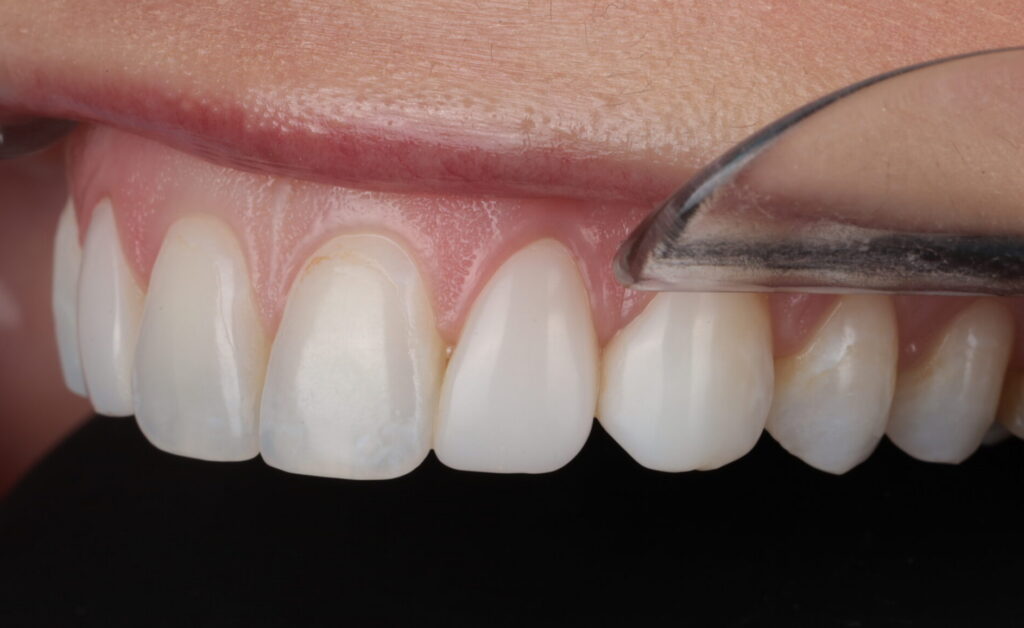
Fig 3
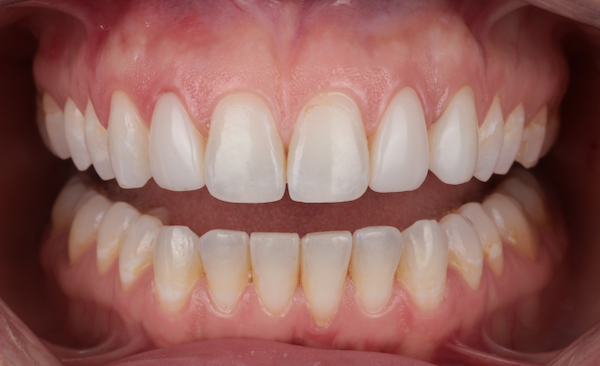
Fig 4

Fig 5
Fig 6
Treatment Procedure
The treatment began with a test fit of the veneers using a selection of colored cements. The veneers were then cleaned in an ultrasonic bath for 3 minutes and air dried. Next, 9.5% hydrofluoric acid was applied precisely for 60 seconds, including the margins, followed by another 3-minute ultrasonic cleaning. Two layers of porcelain primer (silane) were brushed onto the veneers, allowed to sit for 5 minutes, then air dried for 30 seconds. A thin layer of porcelain bonding resin was applied without light curing. The veneers were preloaded with permanent cement and protected under an orange shield after being warmed in the composite warmer. On the tooth surfaces, a plaque indicator was applied followed by fluoride-free pumicing and micro etching with 32% phosphoric acid. The teeth were then etched with 32% phosphoric acid for 30 seconds, rinsed thoroughly for 30 seconds, and 1 to 2 thin layers of All-Bond Universal adhesive were applied, air thinned, and light cured for a minimum of 10 seconds at 800 mW/cm2. The veneers were seated and tack-cured in place to stabilize positioning. Excess uncured cement was then carefully removed prior to final curing as cured cement is highly difficult to remove, especially interproximally. Once excess cement was removed, the veneers were light cured for 20 seconds. A 12-blade scalpel, interproximal saws, and scalers were used to remove any residual cement. Glycerin was then placed over the margins to prevent oxygen inhibition, and a final 20 second cure was done. After rinsing the glycerin, contacts and occlusion were checked, and final radiographs were taken. To prevent damage to the veneer margins, use of a handpiece around the facial margins was strictly avoided. Instead, residual cement was carefully removed using hand scalers and a #12 blade for optimal precision and margin integrity. The total delivery time for 2 veneers including seating, cement cleanup, radiographic verification, and occlusal adjustment was approximately 2 hours.
Outcome and Follow-Up
Two custom-fabricated veneers were successfully delivered, demonstrating excellent marginal adaptation, precise anatomical contouring, and seamless shade integration with the adjacent dentition. The restorations exhibited uniformed esthetic blending with the surrounding teeth, contributing to a natural appearance and enhanced smile symmetry. A comprehensive evaluation of marginal integrity and occlusal relationships was performed, confirming proper interproximal contacts, stable occlusion, and the absence of premature contacts during functional movements. The patient reported satisfaction with both the esthetic and functional outcomes at the time of delivery. A follow-up appointment was scheduled for two weeks post-delivery to allow for further assessment of gingival tissue response, occlusal stability, and overall restoration performance, ensuring the longevity and predictability of the treatment outcome.
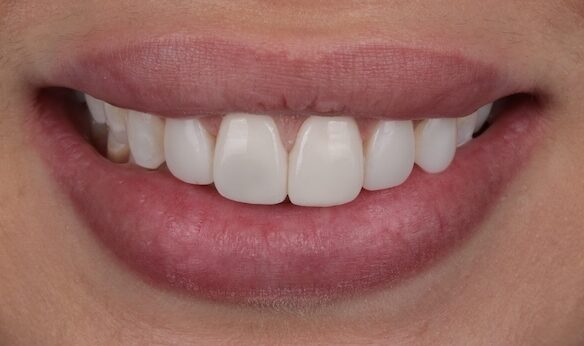
Fig 7
Fig 8
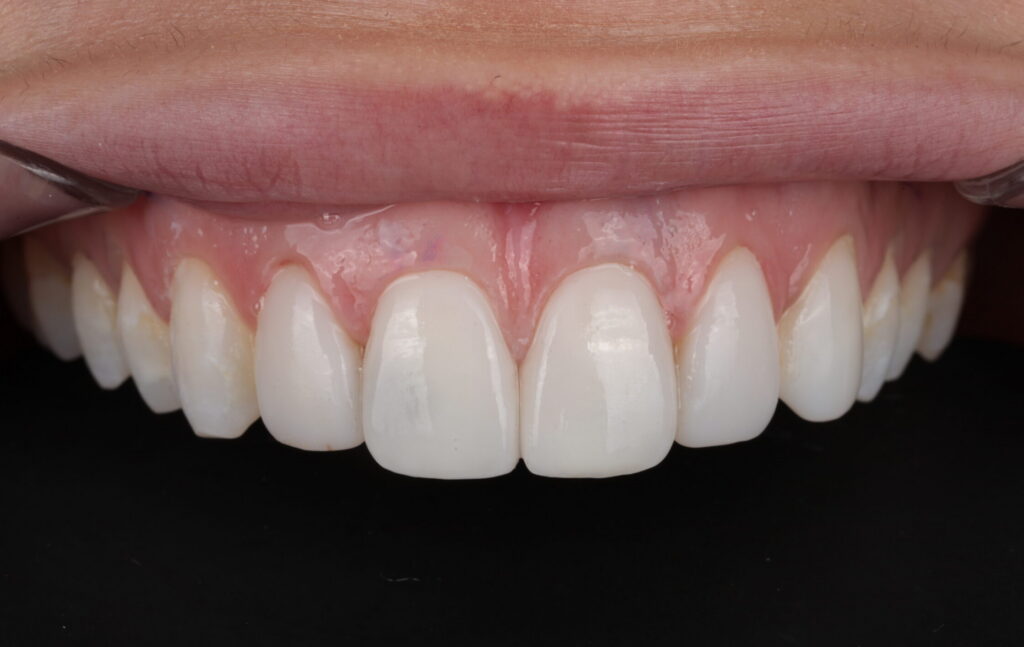
Fig 9
Fig 10
Discussion
Material selection played a critical role in the success of this case. Historically, zirconia has been considered less suitable for ultra thin veneer applications due to concerns related to translucency and adhesive bonding. However, recent advancements in 3D printing technology and surface treatment protocols, including lithium disilicate spray applied to the bonding surface, have expanded the clinical indications for zirconia. These innovations allow for controlled translucency and opacity when indicated, as well as predictable adhesion when proper protocols are followed. In this case, the restorations exhibited excellent marginal adaptation, shade integration, and surface uniformity, supporting the use of UltraThineerzirconia veneers as a viable option in highly conservative esthetic treatments.
From an esthetic perspective, limiting treatment to the central incisors required meticulous shade matching and surface characterization to achieve seamless integration with the adjacent lateral incisors. The final outcome demonstrates that targeted, conservative enhancements to focal esthetic concerns can significantly elevate the overall smile while preserving natural tooth proportions and individual character.
Conclusion
This case report demonstrates that selective, no preparation veneer therapy using UltraThineer, 3D printed zirconia veneers can effectively address localized esthetic concerns while preserving enamel and maintaining natural tooth morphology. By limiting treatment to the maxillary central incisors, improved shade uniformity and surface esthetics were achieved without altering the patient’s existing smile architecture.
The subtle nature of the changes may go largely unnoticed by casual observers. However, to the trained clinician and the patient, the outcome represented a meaningful transformation, resulting in a cohesive smile with no visible shade discrepancies. The addition of minimal layering allowed for correction of minor marginal discoloration without any reduction of tooth structure.
These outcomes highlight the value of a conservative, indication driven approach to esthetic treatment, in which thoughtful material selection and precise clinical execution are essential to success. When used appropriately, ultra thin zirconia veneers provide a reliable solution for addressing a wide range of esthetic concerns, with UltraThineer offering the flexibility to achieve both subtle refinements and more extensive smile improvements while maintainingmaximal preservation of natural tooth structure.
References
- Magne P, Belser UC. Porcelain veneers bonded to enamel and dentin. A biomimetic approach. Quintessence Publishing Co; 2002.
- Guess PC, Schultheis S, Wolkewitz M, Zhang Y, Strub JR. Influence of preparation design and ceramic thicknesses on fracture resistance and failure modes of premolar partial coverage restorations. Journal of Prosthetic Dentistry. 2013;110(4):264–273.
- Blatz MB, Alvarez M, Sawyer K, Brindis M. How to bond zirconia: The APC concept. Compendium of Continuing Education in Dentistry. 2016;37(9):611–617.
